
My previous article dealt with the importance of providing a follow-up program after custom orthotics are dispensed to your patients.
My previous article dealt with the importance of providing a follow-up program after custom orthotics are dispensed to your patients. This article is about keeping detailed notes and the importance of these notes in growing a successful, sustainable orthotic dispensing practice.
It is always my goal to create a lifelong relationship with each of my patients. This creates an opportunity for quality care and continuity of care while creating a positive success rate for you. Proper record keeping involves documenting all of the important findings of my foot and gait examination, my patient’s history and the specifics of the design of the orthotic.
INCREASES SUCCESS RATE AND CONFIDENCE
As I described in part 1, after dispensing orthotics, I make follow-up calls at two weeks and at yearly intervals to collect and record two types of important information: percentage pain relief and percent wear time. This data is valuable in two ways:
Each patient’s percent pain relief is tracked and compared to the average, allowing their progress for each diagnosed condition to be quantifiably tracked. As the database grows, I can determine a success rate for each condition that I treat. This can be used clinically.
Percent wear time is an important statistic because it helps determine if the patient is getting maximum benefit from their orthotics or if compliance, due to lack of ease of use, is a problem. I often find that my patients are not transferring their orthotics from shoe to shoe, which significantly decreases their wear time. This often correlates to their percent pain relief.
Clinical Note
For example, over the last five years that my data collection program his been active, I have documented an average pain relief of 87 per cent for the diagnosis of plantar fasciitis. If my patient comes for a re-examination and has a percent pain relief of 60 per cent, I know that I should be able to do better, even though my patient may be happy. I may need to add something to the design or incorporate some other form of treatment to get them closer to my average of 87 per cent.
INCREASES PATIENT SATISFACTION AND THEIR CONFIDENCE IN ME
When a patient comes in for a re-exam, I can print a re-exam summary so that I have all of their relevant exam and orthotic design information in hand. I can immediately access their previous exam findings, pain location, diagnosis and the types of orthotics they have – they can see that I am organized.
Clinical Note
Recently, one of my patients, who was suffering from severe metatarsalgia with extensive callusing and claw toes, came in for a re-exam. He had been wearing orthotics for years and was getting some relief, but after inspecting his old orthotics, I thought that I could do better. I made him a very soft orthotic with one eighth of an inch underlay between the shell and top cover and, most importantly, I incorporated metatarsal pads to splay apart his metatarsals during his gait cycle. Metatarsal pads come in three thicknesses, 1/16, 1/8 and 1/4 inch. I started with the 1/8 pad and after my two-week follow-up call he felt better but still reported discomfort. I redispensed his orthotics, this time with the 1/4 thick metatarsal pad, and at his two-week follow-up call he reported feeling much better. His changes were logged into my software and upon his re-exam this year, I printed a re-exam summary sheet. I took a look at his callusing and claw toes and compared his present condition to his previous condition, and noted any changes. When asked, he said he was happy with the 1/4 inch pad and the specifics of the previously designed orthotic. All of the information I had gathered and stored and brought with me into the re-exam made me a much better practitioner.
PROVIDES QUALITY ASSURANCE
We have many options to choose from when designing orthotics for our patients, including orthotic length, type of shell material and thickness, and modifications. This variety of options offers great flexibility in designing the correct orthotic for our patients; however, it is very important to know the exact orthotic previously dispensed so that it can be precisely duplicated. Therefore, it helps to maintain a database with meticulous records of each patient’s orthotics. Minor changes can be documented so that the next time the patient is in, we know exactly what was made and that the device they are getting is the right one for them. This results in fewer post-dispensation adjustments, happy patients and more referrals.
Clinical Note
In my practice, patients come in with orthotics from another provider or even from multiple providers. I commonly find that these orthotics vary from pair to pair even if they are from the same provider. It is crucial both to determine the orthotic best suited to the patient and to reproduce that orthotic when they have new pairs made. This way they are walking on a consistent surface in all of their shoes, decreasing the probability that their symptoms will reappear.
INCREASES EFFICIENCY AND SAVES TIME
As I mentioned above, with proper record keeping, I have access to previous physical exam and orthotic design information and do not have to repeat unnecessary exams. Not only does this make me look organized and professional to my patients, it also saves time for both me, and the patient. A re-exam summary sheet is printed and comes with me into the re-exam.
Clinical Note
In my practice, record keeping also includes documenting important findings from my physical exam, the patient’s history and specifics of the orthotic design. Table 1 lists examples of the major things I keep track of in my files for each patient.
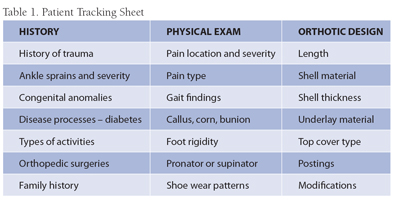 |
IN CONCLUSION
Proper record keeping is very important when building a successful orthotic dispensing practice. It is important to have easy access to this information, which will save you time, make you a better doctor and result in happier patients that continue to refer.
In Part 3, Dr. Dziak will discuss The Importance of Interprofessional Communication and Report Generation. It will appear in the June 2013 issue of Canadian Chiropractor.
In Part 1 of my article I wrote, “In my practice, I schedule re-exams upon insurance eligibility for insured patients, and at three year intervals for uninsured patients.” I would like to clarify that this statement means the following: I have a re-exam frequency of three years – whether patients are insured or not – because this time frame makes sense clinically, and also aligns with most insurance coverage, for those patients who have insurance.
Since orthotics break down over time, all patients require re-exams to have their feet and the condition of their orthotics reassessed. Insurance companies have time frames in their policies because they know that these devices break down and eventually need to be replaced. In my practice, I set time-frames that are clinically sound but that also protect patients from having to pay unnecessary fees throughout their orthotics program. The re-exam may reveal that the patient’s orthotics are in good condition and that another pair is not necessary. Of course, if any patient has an issue before their scheduled re-exam, they are welcome to make an appointment to come see me.
My patients appreciate being called post-dispensation and being scheduled for a re-exam. This way they know that I am committed to ensuring their orthotics are doing what they are designed to do.
 |
|
Dr. Martin Dziak is a chiropractor and certified pedorthist. He is the creator of ORTHOTRACK.ca, a customizable orthotic practice management software. For questions and information, visit ORTHOTRACK.ca , e-mail drmartin@orthotrack.ca, or call 519-954-6100 or 1-888-337-7362.
Print this page