
One of the most important times for a woman to be receiving
chiropractic care is during pregnancy! From the moment of conception
her body goes through a series of remarkable changes. Some are easy to
spot: a growing belly, changes in posture and the changes in gait –
that characteristic pregnancy “waddle.”
Why chiropractic, and how?

|
One of the most important times for a woman to be receiving chiropractic care is during pregnancy! From the moment of conception her body goes through a series of remarkable changes. Some are easy to spot: a growing belly, changes in posture and the changes in gait – that characteristic pregnancy “waddle.”
What we cannot see are the millions of different hormonal changes and chemical reactions occurring both in the mother and the developing baby, all of which are controlled and co-ordinated through the nervous system. Now more than ever, during pregnancy she needs a nervous system that responds immediately and accurately to changing requirements in all parts of her body, and, therefore, she needs a healthy spine!
Chiropractic care prior to conception promotes a more regular menstrual cycle and optimum uterine function.1,2,3,4,5 It prepares the body to be strong, flexible and as balanced as possible to carry the pregnancy. And adjusting women through pregnancy and labour is one of the most rewarding parts of our jobs as chiropractors, because a healthier pregnancy means an easier labour and delivery – a much better transition for the next generation into this world!
 |
|
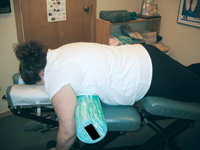
| Figure 1 |
|
 |
|
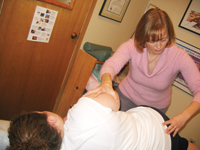
| Figure 2 |
EVIDENCE-BASED PREGNANCY PRACTICE
According to recent studies, chiropractic care may result in easier pregnancy, including increased comfort during the third trimester and delivery, and reduced need for analgesics. In one study, women receiving chiropractic care through their first pregnancy had 24 per cent shorter labour times and subjects giving birth for the second or third time reported 39 per cent shorter labour times. In another study, the need for analgesics was reduced by 50 per cent in the patients who had received adjustments. In addition, 84 per cent of women report relief of back pain during pregnancy with chiropractic care!6,7,8 And because the sacroiliac joints of the pelvis function better, there is significantly less likelihood of back labour (contractions and sharp pain felt in the lower back/sacral area during labour) when receiving chiropractic care during pregnancy.9 Chiropractic care has helped new mothers become more comfortable breastfeeding (posture-wise) as well as to produce more milk.10
MODIFYING CHIROPRACTIC FOR PREGNANCY
As a pregnancy advances, some chiropractic techniques need to be modified for the patient’s comfort and safety. In particular, you should avoid having her lying prone unless you have a table with a drop-away thoraco-lumbar piece, a tilt-up pelvic piece with a roll under her shoulders and/or special pregnancy pillows to accommodate her growing belly (Figure 1). You should be trained in pregnancy-specific techniques, such as Webster or Bagnell techniques, that address uterine constraint (foetal malpresentations). Sacro Occipital Techniques (SOT) blocks work well, especially in a supine position, and I also use an activator extensively. Checking the alignment of the sacrum, pelvic bones, pubic bones, ligaments that support the uterus (e.g., the round ligament), and supporting muscles such as the gluteals, piriformis, thigh adductors and lumbar paraspinals is essential. Additionally, many women will have upper thoracic subluxations from the increasing mass of the breasts in preparation for lactation, lower rib dysfunction from stretching to accommodate the growing belly, as well as cervical subluxations from the shift in the centre of gravity. Ensure that you don’t have the mother lying on her back too long, even with the knees bent (I use a Dutchman’s roll or yoga bolster under the knees for comfort) as lying on the back can put a great deal of pressure on the lumbar spine due to increased lordosis. Lying on the back in the second and third trimester can also cause changes in blood pressure. For some women, it can cause a drop in blood pressure that can make them feel very dizzy; for others, it can cause an unwanted increase in blood pressure.
After checking all of the above, the only side-lying technique that I use in the latest stage of pregnancy is a labour starter or helper. Once mother is ready and there are signs that baby is ready – such as the baby’s head dropping into the birth canal or “lightening”; some ripening or opening of the cervix reported by the midwife or other care provider; post-maturity, or frequent but irregular contractions (regular Braxton-Hicks contractions or practice labour) – I get her to lie on her side, bottom leg bent, while I support her top leg between my knees (Figure 2). I use my thumb or elbow to access the commonly found triggerpoints in the gluteals, piriformis, and hip capsule areas while gently stretching and inferiorly tractioning the top leg with my leg. This technique can be quite intense for the mother-to-be as well as tiring for the practitioner, so watch your own back and make sure the mother-to-be communicates when she needs a break. Generally, I spend three to five minutes on each hip and always assist the mother in getting off of the table, due to the generally weak state of the abdominal muscles in this stage of pregnancy. I have had mothers experience a spontaneous release of the membranes (“waters breaking”) immediately after this technique with speedy onset of labour, so make sure mother and practitioner are prepared for that possibility!
GENERAL WELLNESS IN PREGNANCY
I emphasize that it is vital to ensure she is eating well and getting adequate amounts of the essential nutrients that are needed to sustain a healthy pregnancy. After all, new cells are created to form the two and a half extra pounds of uterine muscle, two pounds of amniotic fluid, placenta (about one pound), a 50 per cent increase in blood volume (approximately four pounds), an extra three pounds in the breasts, about five to eight pounds of extra body stores for pregnancy and breastfeeding as well as the brain, nerves, muscles, tissues, organs and skin of the baby. Additionally, the expectant mother will need to replace many more of her own kidney and liver cells that are used to process the waste of two rather than one. After basic nutritional advice, I also give a list of herbs that are safe, and not safe, to take during pregnancy.
LABOUR
I also recommend some labour comfort techniques including body position and breathing techniques to be used during labour and delivery. Any late-second-stage labour position that denies postural sacral rotation denies the mother and the baby critical pelvic outlet diameter and moves the tip of the sacrum up to four centimetres into the pelvic outlet. In other words, the popular semi-recumbent position that places the labouring woman on her back onto the apex of the sacrum closes off the vital space needed for the baby to get through the pelvic outlet. This delivery position is the main reason so many births are traumatic, labour is stalled and the mom becomes fatigued and overwhelmed by pain, thereby increasing the utilization of epidurals, forceps, episiotomies, vacuum extraction, and caesarean procedure.This is why squatting is the preferred position; gravity works to help and the pelvic outlet can open to a greater degree. Squatting during delivery results in decreased use of forceps and a shorter second stage of labour than the semi-recumbent position!
Moreover, research has shown that coached pushing in the second stage of labour does not improve the short-term outcome for mothers or babies, except when the baby needs to be born as quickly as possible.11 Coached pushing has also been found to potentially increase the amount of pressure on the pelvic floor with subsequent negative consequences such as decreased bladder capacity, less urge to empty the bladder, an overactive bladder muscle, and stress incontinence. Coached pushing also involves “breath-holding” (so-called “purple pushing”) which can be very tiring, reduces oxygen levels in the mother and baby and increases the risk of tearing. An uncoached or a spontaneous second stage of labour allows the mother to work with the uterine contractions and the fetal expulsion reflex and allows the baby to descend without damage as she gently breathes the
baby out.12
Look for Part 2 of this article in the April 2009 issue. Dr. Rosenberg will offer pregnancy exercise tips as well as insight on how to build a pregnancy practice. •
References for Part I
1. Bedell, L. Successful
Pregnancy Following Diagnosis of Infertility And Miscarriage: A Chiropractic
Case Report. Journal of Vertebral
Subluxation Research. December 2, 2003, pp 1-7 www.jvsr.com/access/abstracts.asp?catalogid=186
2. Kokjohn
K, Schmid DM, Triano JJ, Brennan PC. The effect of spinal
manipulation on pain and prostaglandin levels in women with primary
dysmenorrhea. J Manipulative Physiol Ther 15 (5): 279-285 (Jun 1992).
3. Polus BI, Henry SJ, Walsh MJ. Dysmenorrhoea. To
treat or not to treat. Polus, BI, Henry SJ, Walsh MJ. Chiro
J Aust 1996; 26:21-4.
4. Sims L, Lee J. Resolution of Infertility in a Female Undergoing Subluxation-Based Chiropractic Care: Case Report and Review of Literature. (2008, August 6),
pp 1-6. www.jvsr.com .
5.
Sturm B. Fertility Press Release. http://www.drbarbarasturm.com/
6. Berg
G, Hammer M et al. Lower Back Pain During Pregnancy. Obstetrics and
Gynecology. (1988) 71: 701-775.
7.
Diakow P, Gladsby T et al. Back Pain During Pregnancy and Labour. Journal of
Manipulative and Physiological Therapeutics. (1991) Vol 14: 116-118.
8.
Fallon J. The Effect of Chiropractic Treatment on Pregnancy and Labour: A
Comprehensive Study. Proceedings of the World Federation of Chiropractic.
(1991) 24-31.
9. Daly
JM, Frame PS, Rapoza PA. Sacroiliac subluxation: a
common treatable cause of low back pain in pregnancy. Fam Prac Res J 1991;11(2):149-159.
10. Vallone,
S. The role of subluxation and chiropractic care in
hypolactation [case report]. The Journal of Clinical Chiropractic Pediatrics [March 2007; Vol.
8(No.1&2): 518-524]
11.
Schaffer JI, Bloom SL, et al. A Randomized Trial of the Effects of Coached vs.
Uncoached Maternal Pushing During the Second Stage of Labour on Postpartum
Pelvic Floor Structure and Function. American Journal of Obstetrics and
Gynecology. (2005, May) 192 (5): 1692-1696.
12.
Mongan M. (2005). HypnoBirthing®: The Mongan Method: A Natural Approach to a
Safe, Easier, More Comfortable Birthing. (3rd ed.). Health Communications
Inc: Deerfield Beach, FL.
Print this page