
Sample Case
A 40-year-old carpenter presents to the clinic with headaches and low back pain. He informs the doctor that his occupation requires him to work overhead for most of the day, which aggravates his symptoms. The physical exam reveals a decreased range of motion in cervical flexion and in lumbar extension, both of which produce pain at end range. Static and motion palpation reveal subluxations present bilaterally at the occiput, and in the right sacro-iliac joint. The doctor, who is proficient in The Complete Thompson Technique-Minardi Integrated Systems, decides to perform leg length analysis to elaborate on his palpation findings. The doctor finds that the patient presents with even legs in the extended position and even legs in the flexed position. However, when the doctor asks the patient to rotate his head to the right side, the doctor observes that the patient’s right leg pulls short in the extended position. Furthermore, when the doctor asks the patient to rotate his head to the left, the patient’s left leg pulls short. Both radiological and neurological analyses are unremarkable.
 |
|
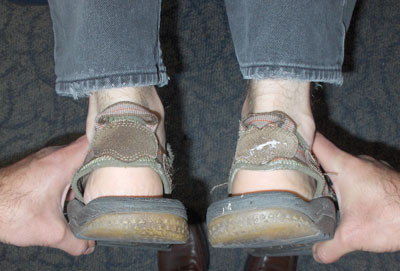
| Photo 1: In BCS presentation part 1, patient presents with even legs in the extended position. |
|
 |
|
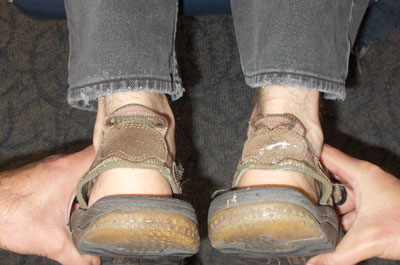
| Photo 2: In BCS presentation part 2, patient rotates head to the right, resulting in the right leg pulling short. | |
 |
|
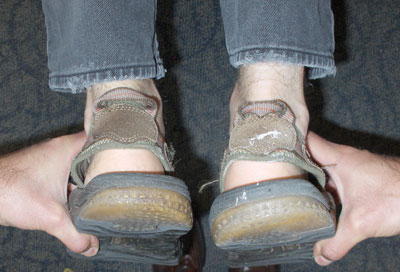
| Photo 3: In BCS presentation part 3, patient rotates head to the left, resulting in the left leg pulling short. | |
 |
|
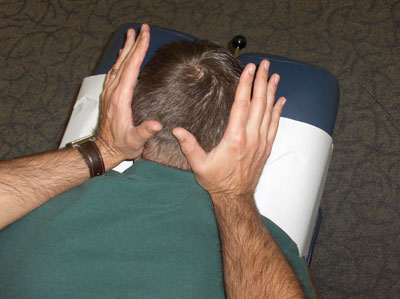
| Photo 4: BCS contacts are displayed. Bilateral thenar contacts are placed inferior to bilateral mastoid processes. | |
 |
|
| Photo 5: Doctor and patient positioning for a BCS are displayed. Note that the doctor is in a fencer stance to focus the thrust in the cephalad direction. |
Sample Case
A 40-year-old carpenter presents to the clinic with headaches and low
back pain. He informs the doctor that his occupation requires him to
work overhead for most of the day, which aggravates his symptoms. The
physical exam reveals a decreased range of motion in cervical flexion
and in lumbar extension, both of which produce pain at end range. Static
and motion palpation reveal subluxations present bilaterally at the
occiput, and in the right sacro-iliac joint. The doctor, who is
proficient in The Complete Thompson Technique-Minardi Integrated
Systems, decides to perform leg length analysis to elaborate on his
palpation findings. The doctor finds that the patient presents with even
legs in the extended position and even legs in the flexed position.
However, when the doctor asks the patient to rotate his head to the
right side, the doctor observes that the patient’s right leg pulls short
in the extended position. Furthermore, when the doctor asks the patient
to rotate his head to the left, the patient’s left leg pulls short.
Both radiological and neurological analyses are unremarkable.
What does this leg length analysis indicate and how do we correct this
problem? In this first instalment of a two-part edition of Technique
Toolbox, I will answer these questions and others, as we take a look at
the Thompson Technique’s Bilateral Cervical Syndrome (BCS) category.
HISTORY
The Thompson Technique was originally created by J. Clay Thompson in the
early 1950s. The technique was created in an attempt to decrease the
force being applied to both the patient and the doctor with each
adjustment. To achieve this goal, Clay drew from his engineering
background and applied Newton’s laws of physics to create the drop-piece
table. The drop-piece allowed less torque to be applied to the patient,
hence, decreasing the force that the doctor absorbed as well. Paramount
to the Thompson technique is the use of leg length analysis, which is
originally credited to Dr. Romer Derefield. Leg length analysis provided
a consistent reference tool to be utilized throughout the adjusting
procedure. Due to the scientific limitations of his era, Clay could not
scientifically explain why the technique worked, even though clinical
trials were validating the technique. Beginning in the late 1990s, and
to the present day, the author has focused on establishing the
neurological and biomechanical rationale underlying the technique and
filling in any gaps that existed within the technique to create a more
scientifically solid system for assessment and adjustment.
Figure 1: The convex occipital condyles sit within the concave lateral masses of atlas. |
|
Figure 2: As the occiput subluxates anterior, it must also travel superior, following the concave surface of atlas. |
BILATERAL CERVICAL SYNDROME
The Bilateral Cervical Syndrome (BCS), despite its name, has very little
to do with the cervical spine. When a BCS is present, this represents
an occiput subluxation, and more specifically indicates that the occiput
has subluxated anterior-superior (AS) bilaterally. Always remember, as
the occiput travels anterior on the lateral masses of atlas, it must
also travel superior as it follows the concave surface of the lateral
masses of atlas. We must always be mindful that anytime the occiput
subluxates anterior or posterior, it must also subluxate superior due to
this concave surface. (See Figures 1 and 2.)
So, how do we find a BCS?
As our sample case described, a patient presents to the clinic with even
legs in the extended position. However, because the BCS is only one of
several problems that can be detected with an even-legs presentation,
the following scenario must be present in order to consider the problem a
BCS.
Step 1: Analysis
Patient presents with even legs in extension. This indicates that the
patient is either subluxation free, or has subluxations present
bilaterally, neurologically producing the even legs presentation.
The doctor has the patient rotate their head to the left, which makes
the patient’s left leg contract (pull short). The doctor then has the
patient rotate their head to the right, which makes the patient’s right
leg contract (pull short). (See Photos 1 to 3.)
If this exact analysis occurs, this confirms that the primary
subluxation is a BCS, indicating that the occiput has subluxated AS
bilaterally.
Because the legs pull short with head rotation, this rules out the
possibility that the patient is subluxation free. If no subluxations
existed, then head rotation would have made no change to the even-legs
presentation.
Step 2: Correction – Classic Thompson Prone Adjustment (See Photos 4-5)
There are several ways of correcting this subluxation. The following is the Classic Thompson Adjustment.
- Doctor: Either side of table.
- Patient: Prone. Chin tucked. Mouth closed.
- Table: Cervical piece in the ready position, and flexed.
- Contact: Bilateral thenars on the inferior aspect of the mastoid processes.
- LOC: I-S, and slightly P-A to initiate the drop piece. Thrust is a sweeping motion.
It is important for the doctor to remember that in order for this
adjustment to be performed properly, four elements must be incorporated:
- tremendous speed must be generated;
- a well-functioning drop piece must be used;
- the thrust should never be focused into the headpiece, as this will injure the patient;
- the focus of the thrust should be concentrated cephalad, with only enough P-A pressure to initiate the drop piece.
Flexing the headpiece and having the patient tuck their chin allows the
doctor to place the occiput in the opposite direction of the subluxation
pattern. This facilitates a biomechanically advantageous position prior
to correction.
Following the adjustment, the doctor rechecks the patient’s leg lengths
and notices that the patient is no longer presenting with even legs. At
this point the patient has a contracted (short) right leg in the
extended position, and when the doctor lifts the patient’s legs to 90
degrees, he notices that right leg continues to pull short.
What does this new leg length analysis indicate? Did the doctor do
something wrong with the occiput adjustment? Are there other
subluxations that now need to be addressed and corrected? I will answer
these questions and more in our next issue of Technique Toolbox. In the
meantime, if you would like to learn more about this technique, please
go to www.thompsonchiropractictechnique.com.
Until next time . . . adjust with confidence.
Print this page