
A doctor of chiropractic can potentially be found in a variety of
clinical settings. Within these settings, patients may present with
concerns ranging from low back pain, to musculoskeletal injuries, to
overall health and wellness concerns.
A doctor of chiropractic can potentially be found in a variety of clinical settings. Within these settings, patients may present with concerns ranging from low back pain, to musculoskeletal injuries, to overall health and wellness concerns.

|
Regardless of the setting and patient presentation, and notwithstanding the chiropractor’s practice vision and philosophy, the adjustment remains at the crux of the chiropractic approach. The routines and procedures that surround and support the act of administering an adjustment vary between chiropractic practices.
Elements in common may be certain assessment protocols – including imaging – and prescribing exercises. Arguably, the perspective from which these are undertaken can, in many situations, either contribute to a successful outcome or impede optimal patient care. Although many factors come into play – including co-morbidities and patient participation – understanding the client’s issues well and targeting all aspects of intervention to this picture can help solidify a beneficial experience for the patient.
 |
|
| Dr. Stuart McGill is a professor of spine biomechanics at the University of Waterloo in Ontario. |
Dr. Stuart McGill is a proponent of this strategy. Dr. McGill is a professor of spine biomechanics at the University of Waterloo in Ontario and consultant for a number of elite athletes and patients with difficult musculoskeletal issues relating to the spine and core musculature. He has written a number of textbooks pertaining to back health and has published several hundred scientific articles in his field. Dr. McGill’s approach is to harness the findings from basic science and clinical investigation of biomechanical aspects of pain and performance to build an evidence-informed approach to assessment and corrective exercise design. It is his opinion that the doctor who is able to fine-tune a critical and tailored approach addressing core causes first and progressively building toward the full gamut of that client’s potential will facilitate the most favourable outcomes.
In the following interview, Dr. McGill discusses some of his findings, and the strategies they have given rise to, with Canadian Chiropractor magazine. The information here is meant to outline an evidence-informed approach to assessment and exercise design that is individual, targeted to core causes, progressive in its administration, and holistic with an eye on long-term injury prevention. These strategies can be tailored to apply to any patient, ranging from those with lifestyle-related back pain to elite athletes striving for optimal performance. As well, they begin with something as seemingly simple as optimal back health and safety as their ultimate goal.
INTERVIEW WITH DR. MCGILL
Canadian Chiropractor:
You have written about flawed movement patterns leading to cumulative trauma and their contributions to pain and/or an injurious event. You mention that back pain and injury statistics ignore cumulative trauma, as do rehabilitation strategies for pain reduction and return to function. Can you discuss how to incorporate these points into a clinical assessment in order to arrive at an optimal treatment and exercise program?
Stuart McGill: In order to identify, and eliminate, the factors that are contributing to cumulative trauma that eventually cause pain, we assess three elements through provocative testing: these are motions, postures and loads that exacerbate pain, and those motions, postures and loads that take the pain away. If the clinician looks at the patient’s/athlete’s daily life and movement patterns, “perturbing motions” can be identified that are causing tissue strain and pain. From there, the doctor can proceed to perform provocative testing, replicating the postures and loading that can confirm exacerbating habits. That is, you can replicate the pain by having the patient play out different motions, postures and load bearing until it irritates them.
This will help you identify the cause of their pain, whether they are a desk worker or a professional athlete.
For instance, a flexion-intolerant patient who sits in spine flexion at a desk throughout the day is engaging in the activity that is causing pain. If you can identify this, through provocative testing, you can design and test a way to mitigate the problem, for instance, by prescribing a lumbar pillow that reduces flexion. Immediately, their instability is buttressed and much, if not all, of their pain is removed. Activities such as walking, lifting, carrying and pushing can be evaluated in the same manner as the doctor determines the changes needed to remove the pain. Note that these interventions fall along a continuum of stability and mobility. Some do better with muscle bracing and stiffening, and others with mobilization. Now, the doctor can continue with treatment strategies – therapy will have a much higher chance of succeeding if you can remove the patient’s pain through eliminating flawed movement or postural patterns. Similarly, with this patient in the example above, the doctor might want to avoid designing exercise routines that involve flexion.
CC: You write that strength and mobility alone, especially in the spine, without control or endurance can actually increase risk. Mobility is often a prime concern, as well as a goal, for clinicians who are trying to help their patients return to optimal function – for chiropractors, this necessarily includes mobility in the spine.
Can you discuss assessment of mobility and its role in treatment and corrective exercise design?
SM: The spine can be likened to a bending beam – a beam can only be bent back and forth so many times before it starts to crack and fail with the stress/strain reversals. The spine is like this, and even more so for some people. The spine can only tolerate so many bends before it begins to accumulate damage, eventually increasing vulnerability to injury and pain. Through provocative testing, the doctor can decide if the patient requires stabilization of the spine before trying to increase its mobility.
To the chiropractor, this may mean that certain manipulations might not be the best first line of treatment, especially if specific mobility contributes to the patient’s perturbed movement patterns or pain generators. For example, shear instability at a specific segmental level can be tested through a provocative test that also evaluates whether stiffening eliminates the pain. We have shown that this is the best predictor of those patients who will do well with a stabilization approach. In this case, it is more justifiable to first stabilize that patient’s spine – not mobilize it. Conversely, two or three initial adjustments might change spinal dynamics enough to reduce pain and better allow for stabilization and other exercise activities. In addition, mobility elsewhere may be the key in addressing some perturbed movement patterns. But only a thorough assessment of the cause of pain can elucidate this. Mobilization through manipulation, and, similarly, exercise involving excessive back movements, might actually not be indicated for every patient.
In addressing the strength and endurance issue, we have found that exercises to increase strength are not always helpful. Giving a patient with perturbed patterns more strength usually results in more repeat episodes of back pain. However, if they have endurance first, so that they are able to repeat tasks with perfect form to avoid the pain mechanism, they will be able to use their newfound strength productively.
So, the order of progression begins with correction of movement patterns establishing appropriate stability/mobility, developing a foundation of endurance and then, finally, strength.
CC: Discuss strategies for stabilization – what does that mean in the context of the spine?
SM: Research shows that, in order for the spine to be stabilized, it must be supported by an orchestra of muscles. The interplay between the spine and core muscles allows for stability in bending, lifting, or whatever the individual needs to do. Research also shows that to focus on a single muscle or muscle group, through targeted exercises, will not provide overall stability. In fact, this approach will create patterns that result in decreased stability.
Power is the product of force and velocity. Spine power must remain low. This is achieved by keeping one of these two variables low. If the speed is high, such as in a golf swing, then the spine muscle forces must be low. Or if the spine muscle forces are high, as in lifting a heavy weight, then the velocity of spine movement must be low. Here, power is developed about the ball and socket joints – the hips and shoulders. The spine transfers the power as a stiffened link. We have measured this pattern in some of the most elite athletes in the world – it is a hallmark of high performance and injury resilience. So, the muscles of the torso are different than the muscles of the limbs – they are designed primarily to stop motion, while the limb muscles are designed create it. They need to be trained differently. Great athletes know this. For example, a mixed martial arts athlete needs to build abdominal armour to survive the sport. Tradition may suggest doing a thousand situps per day. But this violates the spine power principle and reduces the volume of tolerable training. Replacing this with the “stir the pot exercise” enhances tolerable training volume and builds an abdominal short-range stiffness spring to enhance performance and minimize the risk of injury. The approach treats the stabilizing musculature as an orchestra.
CC: How should a corrective exercise program be followed? What should the patient be advised to do and how should his/her progress be directed and assessed?
SM: Each individual has his/her own capacity and tolerance where any movement or exercise program is involved. This needs to be determined. Also, many patients fail because they confuse rehabilitation approaches to reduce pain with those that are designed to enhance performance.
Always begin with a dedicated focus to eliminating pain and then morph to performance-enhancing approaches. Take the example of a patient who states their goal is to play golf. Giving them mobilizing exercises will be counter-productive. Build their pain-free patterns first, which will most likely include exercises to enhance control, stiffness, hip external rotation power, etc. Then work on golf-specific mobility. Conversely, consider the low functioning patient who presents unable to take more than five steps without experiencing pain – regardless of how active that patient was. Their tolerance is very low, so that virtually any rehabilitation program will fail – everything results in pain, except that they can take three steps pain-free. So, this individual, noting that their tolerance is five steps, needs to train three pain-free steps every 15 minutes. They are interval training four times per hour. Eventually they will gain enough tolerance so that the doctor can design a rehabilitation program that will be successful in terms of no pain.
Another consideration is the natural progression of loss of certain abilities that occurs with age, even in very healthy individuals. Even elite athletes will lose some abilities as they age! It is important to recognize these progressions, and identify them in the individual when assessing your patient and designing treatment and corrective exercise programs. What is the person’s capacity and tolerance, now? This is a very dynamic variable.
I must also emphasize the importance of maintaining impeccable form within each step of the training or exercise program. This can reap rewards later on in terms of eliminating the repeating of episodic flareups, and allowing the progression of ability beyond what could otherwise be expected.
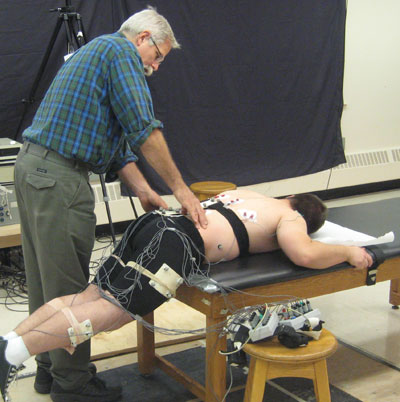 |
|
| Dr. McGill performs a functional assessment while recording resulting muscle activity.
|
SUMMARY
Dr. McGill’s paradigm for assessing back pain and designing treatment and exercise to address it, is based on finding movement pathology that leads to cumulative painful trauma, and removing it. This involves thorough provocative testing. He states that corrective exercises for any aberrant patterns that are identified are the first treatment – teach the patient what causes their pains, and then provide treatment that may be either stabilizing or mobilizing. Mobilizing an unstable joint may result in 20 minutes of pain relief via the modulation of proprioceptors but increases the susceptibility for more instability and pain the next day. He stresses that the causal agent of pain must be removed, in order for the therapy or exercise regimens that follow to be effective. The clinician is advised to design progressive therapy in intervals according to the patient’s current tolerance and capacity, and to ensure pain-free, perfect form has been achieved within each interval before trying to move forward. Performance elements can be safely added when this has been achieved. Finally, Dr. McGill’s evidence shows that the spinal health and stability necessary for enhanced function rely on overall integration of back and core musculature. All strength and ability relies on proximal stiffness of the spine that allows the hips and shoulders to generate power without aberrant spine motion.
This enhances the ability to push, pull, squat, walk and carry, to name a few activities. In other words, it is the key to enjoying pain-free and robust activity.
For more information regarding Dr. McGill, his research and education sessions available to chiropractors, please visit www.BackFitPro.com.
Print this page