
Examining the Lateral Pterygoid Muscle
By Andreo A. Spina BKin DC FCCSS(C)
Features Clinical TechniquesIn view of the increasing emphasis on evidence-based medicine, the
identification and elimination of examination and therapeutic measures
that research demonstrates as unnecessary should represent a high
priority for manual practitioners.
In view of the increasing emphasis on evidence-based medicine, the identification and elimination of examination and therapeutic measures that research demonstrates as unnecessary should represent a high priority for manual practitioners. Many procedures and techniques, however, continue to be taught in educational institutions, and still surface in teaching texts, despite evidence suggesting that they should be altered or eliminated. This leads to the proliferation of incorrect or redundant procedures, and their associated dogma, to new practitioners.
Such is the case regarding examination and treatment of temporomandibular joint disorders (TMD). Historically, examination of this area has included observation of mandibular gait, orthopedic examination, range of motion measures, as well as both extra oral and interior palpation. Believed by many to be the most important muscle in the function of mastication, the lateral pterygoid muscle (LPM) is commonly palpated and utilized as an assessment tool, outcome measure, and target of treatment for manual practitioners dealing with TMD.
However, is palpation of this structure even possible?
 |
|
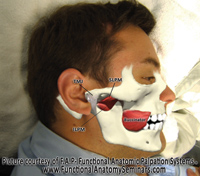
| Figure 1: Temporomandibular joint anatomy demonstrating the superior and inferior lateral pterygoid muscles (SLPM, ILPM), the temporomandibular joint (TMJ), and the buccinator muscles. Note that the overlying temporalis and masseter muscles have been removed.
|
ANATOMY
The lateral pterygoid muscle (LPM) is commonly described as consisting of two distinct heads (inferior and superior). The inferior lateral pterygoid (ILPM), which is up to three times the size of its counterpart, arises from the lateral surface of the lateral pterygoid plate of the sphenoid bone and extends upward, and outward through the infratemporal fossa to its insertion primarily on the anterior and medial aspect of the condylar neck.1 The superior lateral pterygoid (SLPM) originates at the infratemporal surface and infratemporal crest of the greater wing of the sphenoid bone and extends backward, downward, and outward to its insertion primarily on the medial aspects of the pterygoid fovea and the mandibular condyle, as well as the anterior surface of the articular capsule, and the anterior margin of the articular disk (Figure 1).2
The exact insertion of the SLPM, especially its relationship with the articular disk, has been the topic of much debate in the literature. The ideas concerning the settling of the SLPM range from complete insertion into the disk, to partial insertion, to no insertion whatsoever. However, a recent anatomic study by Akar et al. (2009), which examined the muscle’s course in 25 adult human cadaver dissections under 2.5 x loupe magnification, concluded that the main insertions of the SLPM head are not into the disk but into the condyle.1 As discussed below, this finding has obvious implications on the function of the lateral pterygoid muscle.
FUNCTION OF THE LPM
Although small, this muscle of mastication is believed to be the primary muscle affected in temporomandibular joint (TMJ) disturbances.3 But, despite its perceived importance, its function, like its anatomical landmarks, has been subject to debate. The LPM is widely believed to play an important role in control of jaw movement due to the assumed anatomical insertion of the SLPM into the articular disk. During opening, the LPM is believed to contract, and thus the SLPM is subsequently thought to draw the articular disc forward, thereby maintaining the relationship between it and the articular condyle. However, it is now known that the two heads of the LPM are reciprocally innervated so that, during opening of the mouth, the ILPM contracts while the SLPM relaxes. The opposite occurs with closing.4 The disc-condyle relationship is actually maintained by the disc’s strong attachment to the condylar poles such that the disc also moves downward and forward in conjunction with the condyle during opening.1 In addition, Mahan et al. (1983) suggest that the SLPM’s activity of pulling the disc forward is not anatomical, as the SLPM’s major attachment is to the condyle and could pull the disk forward only if the insertion of this muscle is detached from the pterygoid fovea.5
|
|
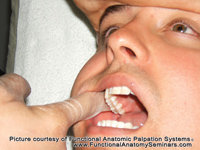
| Figure 2: Palpation technique intended for the lateral pterygoid muscle.
|
PALPATION OF THE LATERAL PTERYGOID
There is little doubt regarding the importance of the LPM in TMJ function.
For a long time, it has been assumed that the inferior belly of this muscle can be accessed near its origin through digital probing, and, thus, its palpation has traditionally been included in study protocols and clinical examinations of the masticatory system.2 In fact, intra-oral palpation of this structure is still included in the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD).6 Attempted palpation of what has been thought to be this structure is commonly done by placing the forefinger, or the little finger, over the buccal area of the maxillary third molar region and exerting pressure in a posterior, superior, and medial direction behind the maxillary tuberosity (Figure 2).
However, as early as 1980, literature such as Johnstone and Templeton’s influential article questioned the ability of a practitioner to palpate this structure.7 Since then, many anatomical and clinical studies have demonstrated the inability to digitally contact the LPM due to its location and surrounding tissues.2
One such study, conducted by Stratmann et al. in 2000, found that “. . . even after maximal impression of the buccal mucosa, a considerable residual distance remains between the ILP muscle and the buccinators fascia indented by the tip of the palpating forefinger.”8 A systematic review carried out by Turp and Minagi (2001) also concluded that: “in the overwhelming majority of cases, palpation of the inferior lateral pterygoid muscle is impossible due to anatomical reasons.”2 The study notes that these reasons include:
- restricted space that does not allow access of the finger (a portion of this potential space is narrowed by the deep tendon of the temporal muscle)
- resistance by the tendinous origin of the buccinator muscle (pterygomandibular raphe)
- resilience of the buccal mucosa due to its close connection to the alveolar gingival that is firmly attached to the maxillary alveolar process
- an obstructing deep origin of the medial pterygoid, which rests on the inferior face of the inferior head of the ILPM.
 |
|
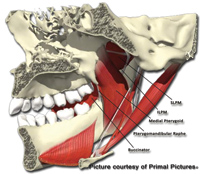
| Figure 3: Medial view of the mastication system. Note the distance between the third molar and the lateral pterygoid muscle. Diagram also shows the buccinator muscle, pterygomandibular raphe, and the medial pterygoid muscle.
|
This may come as a surprise to practitioners dealing with TMDs in their practice, considering that epidemiological studies have shown that patients with these disorders frequently report the most tenderness to palpation of what was thought to be the “lateral pterygoid” muscles in this region. However, one must also consider that the same studies have shown that among individuals not suffering from orofacial pain, the “lateral pterygoid” area is also considerably more tender than other masticatory muscles. If the LPM cannot be implicated for this tenderness, then, one must wonder what the actual cause of the pain on palpation is, if this muscle is, in fact, not accessible.
Various potential structures and mechanisms have been cited to explain this, including:
- stretching of the overlying buccal mucosa
- compression of the buccinators muscle
- palpation of the insertion of the deep tendon of the temporal muscle on the medial surface of the coronoid process
- pressure on fibres of the superficial head of the medial pterygoid
TREATMENT OF THE TMJ AREA
Trigger point treatment, Active Release®, and myofascial release of this area are frequently performed by manual practitioners treating TMDs. As stated above, during treatment of this area, the practitioner is actually contacting muscles of mastication other than the LPM, namely the medial pterygoid and the deep tendon of the temporalis. Therefore, Although specific effects of utilizing these techniques in the management of TMD are actually unknown, it is possible that the benefits clearly attained might be attributable to improvement in these muscle groups. However, studies need to be conducted in order to directly correlate decreased palpatory pain in this region with overall improvements in temoromandibular conditions and to learn what the actual role of these techniques is. In addition, studies are needed to determine the involvement of the structures that are actually palpated in this area in TMD.
Despite our lack of understanding regarding the role of the above-mentioned treatment methods and the involved muscle groups, there is little argument as to the importance of the LPM in overall TMJ function. Thus, it is safe to assume that dysfunction in this muscle group could contribute to temporomandibular joint dysfunction and pain, and necessitate specifically targeted treatment.
 |
|
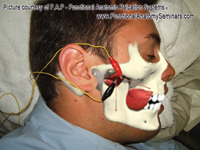
| Figure 4: Medical Acupuncture treatment of the lateral pterygoid.
|
One way that manual practitioners can access and treat the LPM directly is by use of acupuncture (Figure 4). In order to contact the LPM, the needle is inserted into the groove between the condylar and coronoid processes of the mandible, inferior to the zygomatic arch. Placing the patient in a side lying position, then instructing them to open their mouth slightly thereby exposing the aforementioned groove, facilitates easy access to this area. Needle insertion depth is determined by feeling the needle tip contact the lateral pterygoid plate (insertion of the LPM), then retreating slightly. Due to the location of the lateral pterygoid plate, excessive depth of penetration is unlikely and thus the needle insertion is relatively safe and painless for the patient. Although outside the scope of this article, the addition of electroacupuncture stimulation is thought to provide additional neuromodulating effects with intermuscular needle insertions.
Skaggs and Liebenson (2000) published a clinical review describing what they believe to be a method of treating the LPM using a post isometric relaxation stretch technique (PIR).9 While the patient is in a supine position they instruct to “passively open the patient’s mouth and resist the patient’s gentle attempt to poke the chin out for a few sections.” On relaxation they instruct to “take out the slack in the posterior direction of chin retrusion to lengthen the muscle.” The authors recommend repeating the technique for three repetitions.
Medical research can only be considered effective if it changes the practices and/or mentality of its intended audience in a way that, ultimately, benefits patient care. In the case of palpation of the lateral pterygoid muscle, especially in the context of TMDs, chiropractors should embrace this research, in order to better understand the area, and, thus, alter their assessment and treatment practices for these disorders. •
References:
- Akar GC, Govsa F, Ozgur Z. Examination of the Heads of the Lateral Pterygoid Muscle on the Temporomandibular Joint. J of Craniofacial Surg 2009; 20(1): 219-223.
- Turp JC, Minagi S. Palpation of the lateral pterygoid region in TMD—where is the evidence? J Dent 2001; 29(7): 475-483.
- Taskaya-Yilmaz N, Ceylan G, Incesu L, et al. A possible etiology of the internal derangement of the temporomandibular joint based on the MRI observations of the lateral pterygoid muscle. Surg Radiol Anat 2005; 27:19-24.
- Juniper RP. Temporomandibular joint dysfunction: a theory based upon electromyographic studies of the lateral pterygoid muscle. Br J Oral Maxillofac Surg 1984; 22(1):1-8.
- Mahan PE, Wilkinson TM, Gibbs CH, et al. Superior and inferior bellies of the lateral pterygoid muscle EMG activity at basic jaw positions. J Prost Dent 1983; 50:710-718.
- Conti PCR, Dos Santos Silva R, Rosetti LMN, et al. Palpation of the lateral pterygoid area in myofascial pain diagnosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2008; 105:e61-e66.
- Johnston DR, Templeton M. The feasibility of palpating the lateral pterygoid muscle. J of Prost Dent 1980; 44:318-323.
- Stratmann U, Mokrys K, Meyer U, et al. Clinical anatomy and palpability of the inferior lateral pterygoid muscle. J of Prost Dent 2000; 83(5):548-554.
- Skaggs C, Liebenson C. Orofacial Pain. Top Clin Chiropr 2000; 7(2):43-50.
Dr. Andreo A. Spina is the creator and chief instructor of F.A.P. – Functional Anatomic Palpation Systems©, which offers seminars on advanced soft tissue palpation and assessment (www.FunctionalAnatomySeminars.com ). He is also a director of Sports Performance Centres (SPC), sports medicine and high-performance training centres located in the greater Toronto area. Dr. Spina is a fellow of the College of Chiropractic Sports Sciences, a certified medical acupuncturist, and a certified personal training specialist. He can be reached at aas@sportsperformancecentres.com.
Print this page