
Technique Toolbox: Adjusting Secondary Subluxations
By John Minardi BHK DC
Features Clinical TechniquesIn this edition of Technique Toolbox, we continue with our case from
last issue. For clarity, let’s review the sample case that we began
with:
In this edition of Technique Toolbox, we continue with our case from last issue. For clarity, let’s review the sample case that we began with:
 |
|
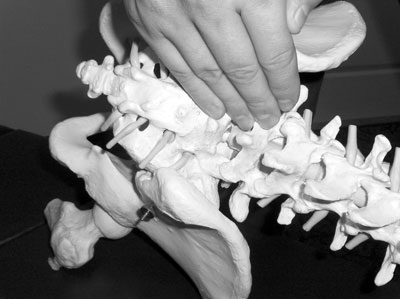
| Photo 1: Contacts for the Split-Leg Lumbar Correction are displayed on a skeletal model. Advertisement
|
Sample Case
A 35-year-old office worker presents to the clinic with neck pain, low back pain and general fatigue. He informs the doctor that he has had the same office job for the past 10 years, and finds himself in front of his computer for hours.
 |
|
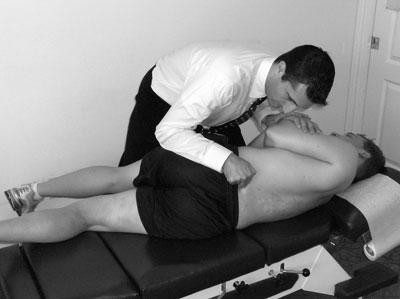
| The contacts for the Split-Leg Lumbar Correction are displayed on the patient.
|
Physical examination reveals anterior head carriage and a flexed thoracic posture. Furthermore, static and motion palpation detects subluxations present at C5 and L5 on the right. The doctor is proficient in The Complete Thompson Technique-Minardi Integrated Systems and performs leg length analysis. The leg check shows a short right leg in the extended position, and a short right leg in the flexed position. The doctor instructs the patient to rotate his head to the left, which balances the legs in the extended position. The doctor then instructs the patient to rotate his head to the right, which keeps the legs unbalanced. Neurological and radiological examinations are unremarkable.
In our last issue, we discussed how you would assess and correct for a cervical syndrome, which is a primary area of subluxation. We concluded by stating that following correction of the cervical subluxation, the legs became balanced in the extended position, but that the patient still presented with a short right leg in the flexed position. What does this mean? Are there other subluxations present? In this edition of Technique Toolbox, we will answer these questions, as we continue with our case.
Following correction of a cervical subluxation, if the leg continues to pull short, the doctor would then analyze and adjust the pelvis. However, sometimes the pelvis is not subluxated, leading the doctor to then assess and correct a secondary area of problem, that is, the lumbar spine.
Analysis
Step One: The patient will present with a contracted leg in extension. In flexion, the contracted leg balances or stays short.
- In many cases, a lumbar subluxation is secondary to an original anterior inferior (AI) sacrum subluxation, and this is the reason that the leg length analysis is identical. When this is the case, the doctor would initially correct for the AI sacrum subluxation, as discussed in a previous issue, then continue to correct the lumbar subluxation.
- The only exception to the above statement is if the lumbar subluxation occurred, or remained, independent of an AI sacrum. When this is the case, the doctor will encounter the short-to-short leg length phenomena described previously – however, no tender points will be present.
- Lack of tender points rules out an AI sacrum subluxation and points to a lumbar subluxation. In this case, the doctor would not adjust the sacrum, but would rather move directly to the lumbar spine.
Step Two: Static palpation reveals spinous deviation ipsilateral to the AI sacrum (original short-leg side).
- Palpation will also reveal erector spinae tonicity and aberrant lumbar interspinous spacing as well as localized edema in chronic cases.
- Motion palpation of the lumber spine reveals a lack of proper joint movement, further confirming the presence of the lumbar subluxation.
Biomechanics
- L5 subluxates posterior due to the coronal orientation of the facet joints between L5 and S1. Due to the fact that the L5 facets are positioned posterior to the S1 facets, the only direction that the lumbar spine can move initially is posterior.
- The only two exceptions to this rule are facet tropism or a spondylolisthesis. These allow L5 to translate anterior; however, these are cases are much more unusual and will be discussed at a later date.
- Following the posteriority, L5 then rotates spinous toward the side of the original AI sacrum subluxation. As the sacrum subluxates AI, it will cause the lumbar spine to rotate with it due to the anatomical position of L5 on S1.
Step Three: Correction: Lumbar Split-Leg Adjustment (see Photos 1 and 2).
The lumbar spine Split-Leg Modification Adjustment was created as an alternative for doctors or patients who prefer the side posture adjusting position. However, these individuals also prefer to use the drop piece mechanism to their advantage.
- Patient: Side posture with the involved side down. Top leg straight and draping off of the table.
- Doctor: Side of table.
- Table: Lumbar piece in the ready position.
- Contact: Pisiform or fingertips on the mamillary process.
- Stabilization: Elbow of patient.
- LOC: P-A. Repeat three times.
For the adjustment to be most effective, the doctor must thrust through the contact, using a slight body drop to initiate the drop piece mechanism.
- The P-A thrust corrects for the posteriority and the unilateral contact will correct for the rotation.
- Both of these are aided by the drop piece, which will increase the speed of the adjustment.
If the doctor does not have access to a drop table, then he/she should perform the exact adjustment described manually.
It is important for the doctor to note that a side posture “lumbar spinous pull” adjustment will only correct for the rotational component of the subluxation, not for the posteriority. Therefore, a “lumbar spinous pull” should not be performed for this subluxation, as it is not the most effective adjustment to utilize.
If a side posture manual adjustment is preferred over the one described, then the doctor must use a “lumbar push” adjustment, contacting the mamillary process contralateral to spinous deviation. This adjustment will correct for the rotation and posteriority of the subluxation, which will produce the desired result.
Following correction of the lumbar spine, the patient in our sample case displayed balanced legs in both the extended and flexed position, and stayed balanced with head rotation. This indicated that the patient was now subluxation free.
As usual, I have only scratched the surface with Thompson Technique – Minardi Integrated System analysis and correction. If you would like to learn more, please go to www.thompsonchiropractictechnique.com or e-mail me at johnminardi@hotmail.com.
Until next time . . . adjust with confidence!
| Erratum Please note that there are two inconsistencies in my article on the anterior humeral subluxation, published on pages 12-14 of the June 2012 issue of Canadian Chiropractor. The first: The text for Photo 3 reads, “Alternative correction if the patient cannot flex shoulder and arm” – yet the image shows the patient with a flexed shoulder and elbow. The second: the subhead “Step Two: Correction: Supine Anterior Humerus Adjustment” directs readers to Photos 1 and 2. The text states that the patient position is supine, with the affected shoulder and elbow flexed to 90 degrees…yet, in Photo 2, the shoulder and elbow are straight. Please note that these tag-lines were misplaced to the opposite pictures. |
Dr. John Minardi is a 2001 graduate of Canadian Memorial Chiropractic
College. A Thompson-certified practitioner and instructor, he is the
creator of the Thompson Technique Seminar Series and author of The
Complete Thompson Textbook – Minardi Integrated Systems. In addition to
his busy lecture schedule, Dr. Minardi operates a successful private
practice in Oakville, Ontario. E-mail johnminardi@hotmail.com, or visit www.ThompsonChiropracticTechnique.com .
Print this page