
Technique Toolbox: Double cervical lock adjustment
By John Minardi BHK DC
Features Clinical TechniquesA 40-year-old engineer presents to the clinic with neck pain, low back stiffness and general fatigue.
A 40-year-old engineer presents to the clinic with neck pain, low back stiffness and general fatigue. He informs the doctor he has had the same job for the past 10 years, and finds himself in front of his computer for hours. Physical examination reveals anterior head carriage and a high left pelvis. Furthermore, static and motion palpation detect subluxations present at C3 left, as well as C5 and S1 on the right. The doctor is proficient in the Complete Thompson Technique-Minardi Integrated Systems, and performs leg length analysis. The leg check shows a short right leg in the extended position, and a short right leg in the flexed position. The doctor instructs the patient to rotate his head to the left, which balances the legs in the extended position. The doctor then instructs the patient to rotate his head to the right, a movement which also balances the legs in the extended position. Neurological and radiological examinations are unremarkable.
 |
|
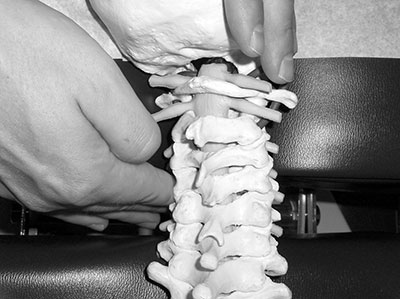
| The DCL contacts are displayed on the skeletal model. This would be done bilaterally, first at the superior nodule and then at the inferior nodule on the opposite side. Advertisement
|
What do these leg length findings indicate? What should be analyzed first? What needs to be corrected and how do we correct the problem?
The cervical spine is considered a primary subluxation area and one of the most powerful areas to correct in our patients. When adjusted properly, the cervical correction has tremendous effects. With this in mind, the cervical syndrome is the initial problem that a Thompson practitioner must rule in or out with the patient. The following procedures are required to detect and correct the double cervical lock subluxation:
Step 1: Analysis
- Patient must present with a contracted leg in extension.
- Doctor instructs the patient to turn his or her head to the left then to the right.
- In order for a double cervical lock to be diagnosed, the patient’s legs must balance upon head rotation to both sides. If the patient’s legs balance with head rotation only to one side, this would be labelled a cervical syndrome, and would be a different subluxation.
- As in our sample case, if the patient presents with a contracted right leg and head turning to both the left and the right balances the patient’s legs, then this would point to a possible double cervical lock subluxation. This indicates that two independent cervical subluxations are present: one subluxation on the left side of the cervical spine and one on the right side.
- The doctor must note that the patient’s legs must balance 100 per cent with head rotation for the double cervical lock to be present. If the legs partially correct but do not become completely balanced, this would not be considered a double cervical lock and the doctor would continue to the next area of concern prior to adjusting the cervical spine. Following correction of that area, the doctor will revisit the cervical spine by having the patient turn their head to both sides again to verify if the double cervical lock is now present.
- Palpate along the lamina-pedicle junction from C2 to C7 on both the left and right sides, feeling for a tender “pea-shaped” nodule. This nodule is an inflamed facet capsule, which is extremely tender due to inflammatory mediators gathered within the capsule. It is important to locate the capsule itself and not simply contracted musculature in the cervical region. A simple test to confirm the capsule is the “roll test.”
- When the doctor finds the pea-shaped nodule, he rolls the mass between his fingers up and down and side to side. If the mass can be rolled, then the doctor is on muscle. The facet capsule is located beneath this muscle mass, is firm and does not move. This nodule confirms the location of the cervical subluxation.
- In our example, we found a nodule at C3 on the left, and C5 on the right.
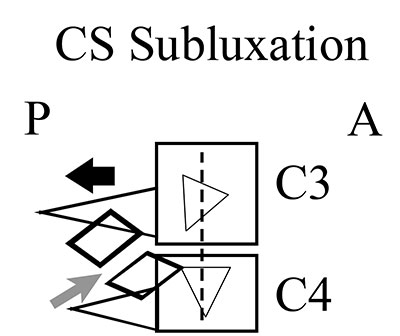
- Figure 1 demonstrates the biomechanics involved in a double cervical lock anywhere from C2 through C7. Note that the affected segment subluxates posterior, and rotates spinous process away from the side of the nodule (indicated by the black arrow). The subluxation pattern stretches the facet, causing inflammation to build and results in a palpatory nodule within the facet joint (indicated by the grey arrow).
 |
|
| Figure 1: CS Subluxation
|
Based on these biomechanics, the doctor must correct for both the posteriority and rotational components of the subluxation. This is accomplished by the doctor thrusting P-A, perpendicular to the facet, and parallel to the disc plane. To achieve this, the doctor’s line of correction must change throughout the cervical spine to compensate for a patient’s natural cervical lordosis. Therefore, in superior cervical segments, the line of correction will be cephalad, and will gradually become caudad with each inferior segment.
Step 2: Double cervical lock adjustment
- Doctor: side or head of table.
- Patient: prone.
- Table: cervical piece in the ready position.
- Contact: MCP or PIP joint on the LPJ (location of nodule). Always adjust the superior segment first, followed by the inferior segment. In our sample case, the C3 vertebra would be adjusted first, followed by C5.
- Stabilization: opposite side zygomatic arch or parietal bone.
- LOC: P-A, L-M perpendicular to the facet joint and in line with disc plane.
- The anterior to posterior thrust corrects for the posteriority of the subluxation, and the unilateral contact on the lamina-pedicle junction corrects for the rotational component involved. Thus, the doctor will be thrusting into the patient’s natural cervical lordosis, restoring the affected segment back into a normal position.

|
|
| The DCL contacts are displayed on the patient.
|
After the cervical subluxation is corrected, the legs become balanced in the extended position, but still present as a short right leg in the flexed position. What does this mean? Are there other subluxations present?
We will answer these questions in our next edition as we continue on with our sample case.
Until next time… adjust with confidence.
Dr. John Minardi is a 2001 graduate of Canadian Memorial Chiropractic College. A Thompson-certified practitioner and instructor, he is the creator of the Thompson Technique Seminar Series and author of The Complete Thompson Textbook – Minardi Integrated Systems. He can be contacted at johnminardi@hotmail.com. For more information visit, www.thompsonchiropractictechnique.com .
Print this page