
SAMPLE CASE
A 35-year-old construction worker presents to the clinic with severe headaches. He informs the doctor that the headaches began two years ago with the start of his job, and have been consistently present ever since. He explains to the doctor that his occupation requires him to operate a jack-hammer for 10 hours a day, causing him to look downward toward the pavement the entire time. His job also requires him to be in a constant state of tension throughout his body, in order to stabilize the jackhammer throughout the intense vibration that the tool generates.
SAMPLE CASE
A 35-year-old construction worker presents to the clinic with severe headaches. He informs the doctor that the headaches began two years ago with the start of his job, and have been consistently present ever since. He explains to the doctor that his occupation requires him to operate a jack-hammer for 10 hours a day, causing him to look downward toward the pavement the entire time. His job also requires him to be in a constant state of tension throughout his body, in order to stabilize the jackhammer throughout the intense vibration that the tool generates.
 |
|
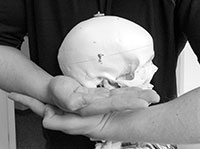
| Photo 1: Seated occiput lift adjustment contacts are displayed on the skeletal model | |

|
|
| Photo 2: Seated occiput lift adjustment contacts are displayed on a patient. Advertisement
|
Physical examination reveals anterior head carriage and a flexed thoracic posture. Furthermore, range of motion testing reveals that the patient has difficulty extending the head and neck. Motion and static palpation reveals that the occiput is subluxated posterior bilaterally, with subsequent tension in the sub-occipital muscles bilaterally. It is also interesting to note that palpation along the sub-occipital muscles aggravates the patient’s headaches immediately during the examination. Neurological and X-ray analysis are unremarkable.
Have you ever encountered an occiput subluxation in your office and had a hard time correcting it with traditional adjustments? Have you noticed that patients with occipital subluxations often have signs of poor health, including headaches? Why are these issues such common themes with these types of subluxation patterns? In this edition of Technique Toolbox, I will answer all of these questions and more as we analyze a common occipital subluxation, and the seated occipital lift adjustment.
OCCIPUT SUBLUXATIONS AND SIGNS OF POOR HEALTH
I must begin by stating that regardless of the area of subluxation, anyone who is subluxated will exhibit signs of poor health. Those signs will simply vary from individual to individual.
As was stated earlier, many patients who have occipital subluxations, whether they are unilateral or bilateral, tend to suffer from headaches. These symptoms are often due to the subluxated occiput’s influence on the rectus capitis posterior minor. This sub-occipital muscle originates at the occipital nuchal line and inserts to the posterior tubercle of atlas. What makes the rectus capitis posterior minor muscle unique is that it also has attachments to the posterior atlanto-occipital membrane, resulting in a direct influence on the nervous system. Current research suggests that a soft-tissue bridge connecting the rectus capitis posterior minor to the posterior atlanto-occipital membrane was present in the majority of cadaver specimens examined, and was reflective of normal anatomy.1 The results of this research provide the doctor with the indication of a strong anatomical connection linking subluxations in the atlanto-occipital region with patient headaches.
Other research has also suggested an anatomic relation between the rectus capitis posterior minor and the dura mater at the atlanto-occipital junction. The researchers stated that every specimen examined exhibited the connection, and that the fibres were positioned to resist movement of the dura toward the spinal cord.2 These studies reinforce the importance of properly assessing and correcting occiput subluxations. When the occiput subluxates, it will have a direct influence on the rectus capitis posterior minor, which will lead to distortions of the dura and the atlanto-occipital membranes due to its connective tissue attachments. This distortion may lead to a variety of symptoms, including headaches, all of which can be eliminated once the subluxation is detected and corrected.
ANALYSIS
The patient in our sample case has a bilateral posterior occiput as determined through motion and static palpation. However, the seated lift adjustment requires that the occiput be adjusted one side at a time. Therefore, the doctor must perform a simple clinical analysis to determine which side to start with. Even though the occiput is subluxated bilaterally, there is always a dominating side of subluxation and that is the side that the doctor must start with.
- The doctor stands behind a seated patient.
- Instruct the patient to turn their head to the left and then to the right.
- On the side to which the patient has the most range of motion (can turn the farthest) is the position in which the doctor will start this adjustment. For example, if the patient can turn their head farthest to the right, the doctor will take his/her contact with the patient’s head turned to the right, and will be contacting the patients left mastoid process. The doctor will then repeat this adjustment with the patient’s head turning to the left, hence contacting the right mastoid.
In our example, the doctor started with the most affected side (left occiput) as the subluxated occiput was the reason that the patient could not turn as far to that side.
CORRECTION: MODIFIED SEATED LIFT – (See Photos 1 and 2)
- Doctor: standing.
- Patient: seated, head turned to the side of most motion.
- Contact: hypothenar contact on opposite mastoid process.
- Stabilization: reinforce contact hand.
- LOC: superior distraction. Repeat on opposite side.
It is important for the doctor to ensure that the patient’s jaw is closed. This prevents the patient’s teeth from chattering, or the patient from biting their tongue during the adjustment. The doctor must also avoid contact with the temporomandibular joint (TMJ), to prevent subluxating it indirectly. Furthermore, in order for this adjustment to be effective, the doctor must use his/her legs to distract the occiput from atlas prior to the thrust. Since rectus capitis posterior minor is most likely involved, it is also beneficial to refer the patient for soft-tissue treatment to assist with the dural tension.
As usual, I have only scratched the surface of occipital subluxations and corrections. This distraction of the occiput from the lateral masses of atlas is beneficial for both posterior and anterior occiput subluxations, but is by no means the only method of correction. If you have any questions, e-mail me at johnminardi@hotmail.com.
Until next time . . . adjust with confidence.
REFERENCES
- Hartwell, S. et al. Soft tissue connection between rectus capitus posterior minor and the posterior atlanto-occipital membrane: a cadaveric study. Journal of Chiropractic Education. 2006; 20 (1).
- Hack, G. et al. Anatomic relation between the rectus capitus posterior minor muscle and the dura mater. Spine. 1995. 20(23):2484-2486.
Print this page