
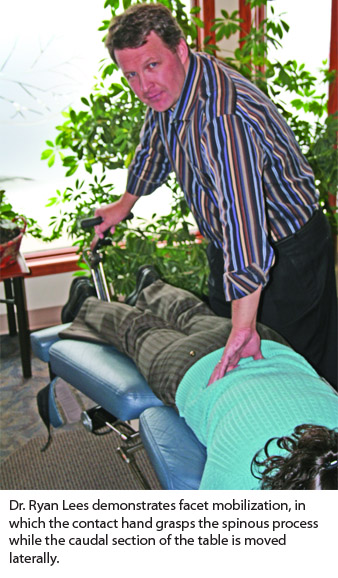
Flexion-distraction system focuses on the biomechanics of the lumbar spine.
 As a rookie doctor, I well remem-ber scenarios when a patient would shuffle through the door in an antalgic posture or with pain radiating down one of their legs.
As a rookie doctor, I well remem-ber scenarios when a patient would shuffle through the door in an antalgic posture or with pain radiating down one of their legs.
I’m sure you’ve similarly encountered many patients who could barely climb onto the table, let alone tolerate a side posture adjustment. Admittedly, my experience and adjusting techniques at that time were limited to that of a new graduate as I deduced how best to help these people recover more quickly and completely.
Dr. James Cox, developer of the Cox Decompression Adjustment and Manipulation Technique (Cox Technique), had similar questions early in his career. He tells of adjusting a woman using a side posture lumbar roll and not achieving the outcome he desired or expected. That dramatic experience was the catalyst he needed to begin thinking about a different way to handle patients with lower back pain (LBP), ultimately leading to the development of his technique system. This discussion will be limited to the technique’s application for low back and leg pain, while acknowledging that it also offers a safe and effective approach for neck and arm pain.
At the heart of the technique is a deep understanding of the biomechanics of the lumbar spine and the causes of LBP. According to Dr. Cox, there are two basic causes of lower back pain: the disc and the facet joints. These are related causes, in that a process leads to disc degeneration and facet arthrosis. To better understand what is happening to our patients, the question must be asked, “Which comes first, the disc lesion or the facet irritation?” It is Dr. Cox’s opinion that “the initial change takes place in the intervertebral disc, which later affects the articular facet.”(1)
The initial changes are microscopic tears secondary to bending, lifting or twisting stresses. These microscopic tears will eventually rupture, causing overt annular damage. Because the disc is richly and complexly innervated and because the outer annular fibres appear to be the most pain-sensitive, annular tearing can refer pain to the low back, buttocks, sacroiliac region and the lower extremity even when there is no direct nerve root involvement. In other words, what can often appear to be a simple lumbar strain or a sacroiliac syndrome is actually an injury to the annulus fibrosis. And because the disc does not well tolerate rotational stresses, side posture adjusting may not be the most judicious approach.
Its application is useful for people with disc herniations, facet syndromes, spondylolisthesis, central stenosis, sciatica, and degenerative disc disease.
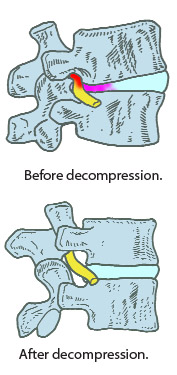 As the decay process continues, the disc will become less and less able to adequately bear compressive loads, and more strain will be borne by the facet joints. Since the facet joints were designed to bear only approximately 20 per cent of the total load, they break down if more is required of them. This increased strain will eventually lead to arthrosis and pain from the facet joints.
As the decay process continues, the disc will become less and less able to adequately bear compressive loads, and more strain will be borne by the facet joints. Since the facet joints were designed to bear only approximately 20 per cent of the total load, they break down if more is required of them. This increased strain will eventually lead to arthrosis and pain from the facet joints.
So how can the Cox flexion-distraction technique deal with these and other problems? First, we need to clearly understand the dynamics of the disc and how it responds to flexion and extension.
When the lumbar spine is put into flexion, a number of important events occur:
• Protrusion of the disc into the intraspinal space is lessened.*
• The ligamentum flavum is stretched, producing reduced bulge into the spinal canal.
• There is stretching of the nerve roots, reducing their cross-sectional area.
• Intradiscal pressure is dramatically reduced.
• Osseoligamentous canal (IVF) area increases by 28 per cent.
* While it is true that the nucleus tends to migrate posteriorly in flexion, the tightening of both the posterior annular fibres and the posterior longitudinal ligament produces a net effect of decreased disc bulge.
The net effect is an increase in the spinal canal and osseoligamentous canal volume and a decrease in the nerve root bulk. These are the primary reasons why flexion-distraction is so effective in instances of disc bulge.
DRAMATIC RELIEF
Care with the Cox Technique can often provide dramatic relief where there are few other effective options. Application of the technique requires a specially designed flexion-distraction decompression table. The table’s caudal section allows movement in flexion and extension as well as lateral bending. This is a hands-on technique with the doctor contacting the patient at all times. The basic premise is for the doctor’s contact hand to stabilize the segment above the level of the lesion while the other hand applies movement to the table. Tissue slack is taken up by dropping the caudal section until tautness is sensed. From this point, the table is alternately dropped a further one to two inches and raised up back to the point of tautness in a rhythmical push-pull pumping action. Each pump lasts about four seconds, with five or six repetitions. This 20-second flexion-distraction session is repeated three times. There are several protocols that can be used, depending upon whether you are dealing with an acute disc or a facet problem. Recent cadaveric studies have demonstrated that the flexion pumps dramatically reduce intradiscal pressure and actually create an intradiscal vacuum. This vacuum helps to draw the nucleus back to its more central location and also draws nutrients in to the disc through the end-plates to aid in healing.
These adjustments should be supplemented with specific home exercises, and the patient receives instruction to avoid sitting, bending, lifting and twisting.
So what kind of results can one expect from using this technique? Clinical research has found that the average number of days to maximum improvement is 29 and the average number of visits is 12, regardless of the specific diagnosis.(2) Maximum improvement was defined as either three months of care, pre-injury status, or 100 per cent relief.
This is a technique that is based on mountains of basic science and clinical research, with several government-funded projects completed or currently underway in the United States.(3-7) It is a system that has proven invaluable in my practice for a wide variety of low back issues. Its application is useful for people with disc herniations, facet syndromes, spondylolisthesis, central stenosis, sciatica, and degenerative disc disease.
Patients with difficult problems are welcomed in my clinic where the utilization of this well-researched technique offers them a tremendous opportunity for recovery.•
References:
Cox JM. Low back pain: mechanism, diagnosis and treatment. Fifth edition. Williams & Wilkins, 1990:68.
Cox et al. Topics in clinical chiropractic, 1996:3(3).
Gudavalli MR et al. A randomized clinical trial and subgroup analysis to compare flexion-distraction with active exercise for chronic low back pain. Eur Spine J 2005; 15:1070-1082.
Gudavalli MR, Cox JM, Baker JA et al. Intervertebral disc pressure changes during the flexion-distraction procedure for low back pain. Abstract from the proceedings of the International Society for the study of the lumbar spine, Singapore, 1998.
Gudavalli MR. Comparison of medical conservative care to chiropractic flexion distraction care of neck pain. Currently underway at Palmer Center for Research. No released outcomes yet.
Meeker W. Comparsion study of flexion distraction, chiropractic side posture, and medical care of elderly patients’ low back pain. Currently underway at Palmer Center for Research in cooperation with the University of Iowa. No released outcomes yet.
Meeker W. Predicting low back pain patients’ response to spinal manipulation (chiropractic side posture and flexion distraction). Currently underway at Palmer Center for Research. No released outcomes yet.
Print this page